About 30% of people with depression don’t improve with medication. Many start looking for something different. TMS therapy may be worth considering.
Transcranial Magnetic Stimulation (TMS) is a non-invasive, FDA-approved therapy that uses targeted magnetic pulses to stimulate underactive areas of the brain linked to mood regulation. No drugs. No systemic side effects. Just science-backed treatment with high success rate in treatment-resistant cases.
But how do you get TMS? Is it covered by insurance? Do you need a referral?
Who Is a Candidate for TMS?
TMS is for people who don’t get better with medications or therapy. Many try antidepressants but either feel no change or deal with unwanted side effects. This drug-free treatment works for those who need something different.
Key Eligibility Criteria:
- Treatment-resistant depression (TRD): The FDA approves TMS for individuals who have tried at least one but often two or more antidepressants without improvement.
- Generalized Anxiety Disorder (GAD): TMS may help when anxiety is persistent and unresponsive to medication.
- Obsessive-Compulsive Disorder (OCD): Approved for OCD treatment when traditional options fail.
- PTSD in veterans and civilians: Research shows that TMS can help regulate brain activity associated with trauma response.
- Chronic migraines: The FDA has cleared TMS for migraine relief, especially for those resistant to medication.
- Patients with medication side effects: Many people discontinue antidepressants due to weight gain, fatigue, sexual dysfunction, or emotional numbness. TMS gives people another way to treat their symptoms.
- TMS for Teens and Young Adults: FDA approves TMS for teens and young adults ages 15 to 21 with Major Depressive Disorder (MDD). Studies are still looking into its use for younger children. TMS is not yet widely available for those under 15.
- People without neurological conditions or implants: A history of seizures or metallic implants in the skull may disqualify candidates due to the nature of magnetic stimulation.
Who Might Not Be Eligible?
- Individuals with epilepsy or frequent seizures.
- Individuals with ferrous metallic implants in the head and neck including cochlear implants, cerebral coils, etc.
How Does the TMS Process Work?
TMS follows a structured, science-backed process. Treatment happens over multiple sessions. Each session is adjusted for the person.
1. Initial Consultation and Assessment
- Conducted by a physician.
- Reviews medical history, current symptoms, and past treatment failures.
- Determines whether TMS is appropriate and discusses insurance coverage or self-pay options.
2. Motor Threshold Mapping (Baseline Calibration)
- The treatment begins with a motor threshold test to personalize stimulation intensity.
- A TMS device sends pulses to the prefrontal cortex.
- The goal is to find the lowest stimulation level that causes a motor response (typically a hand twitch).
3. Treatment Sessions (3-20 Minutes Per Session, 5 Days a Week)
- The patient sits comfortably while the device delivers repetitive magnetic pulses to targeted brain regions.
- No sedation or anesthesia required. Patients remain awake.
- Sessions typically last 3-20 minutes over 6-7weeks, totaling 30-36 sessions. Most indications covered by insurance are 36 sessions but if there is no significant response by week 5 then we can apply to the insurance to request a treatment extension.
- Side effects are minimal—some experience mild headaches or scalp discomfort, which subside.
4. Tracking Progress and Adjustments
- Patients often notice mood improvement within 2-4 weeks.
- Some individuals need adjustments to stimulation intensity based on their response.
- Depression remission rates with TMS range from 60-70%, with significant symptom reduction in others.
5. Maintenance and Follow-Ups
- Preservation TMS involves scheduled sessions right after the initial course to help prevent relapse before symptoms return. Maintenance TMS is used later, if symptoms begin to reappear.
- Follow-up care with a doctor helps sustain long-term mental health improvements.
How to Find a TMS Provider Near You
Not all TMS clinics offer the same level of expertise. Choosing the right provider ensures safety, effectiveness, and personalized care.
Key Factors to Consider:
- Board-Certified Providers: Ensure the psychiatrist or TMS specialist is certified in TMS therapy and understands psychiatric care.
- Physician-Led Care: Choose a TMS center where evaluations and treatment are overseen by a physician trained in TMS.
- Insurance Coverage & Financing Options: Most insurances cover TMS for depression. Verify coverage before starting treatment. If insurance denies coverage, some clinics offer payment plans.
- Reputation & Patient Outcomes: Read reviews, ask for patient success rates, and choose a provider with proven results.
- Personalized Treatment Approach: Effective TMS therapy isn’t one-size-fits-all. It should be customized based on brain mapping and patient response.
Where to Start Your Search
- Ask your psychiatrist or primary care provider for referrals.
- Search online using “TMS therapy near me” and check clinic credentials.
- Look for TMS specialty centers rather than general mental health clinics.
Is TMS Therapy Safe?
TMS is FDA-approved, research-backed, and safe with minimal side effects. ECT requires anesthesia and may cause memory loss, but TMS does not. Treatment is non-invasive, and patients stay awake.
Clinical Safety Data
- Over 75 clinical trials confirm the safety and effectiveness of TMS.
- About 60-70% of patients experience significant symptom relief.
- Seizures are rare with TMS, affecting under 1:100,000 of patients. The risk is very low, making it a safe treatment.
Common Side Effects (Mild and Temporary)
- Scalp discomfort at the stimulation site (subsides after a few sessions).
- Mild headaches (resolves with over-the-counter pain relievers).
- Tingling or twitching in facial muscles during stimulation (temporary).
TMS vs. Medication: Safety Comparison
- No systemic side effects. Unlike antidepressants, TMS does not cause weight gain, nausea, or sexual dysfunction.
- No withdrawal symptoms. Unlike SSRIs and SNRIs, which require tapering off to prevent withdrawal effects.
- No memory issues or sedation. Unlike ECT, which can cause cognitive impairment.
Long-Term Safety
- TMS has been FDA-approved since 2008, with no long-term risks identified in 15+ years of clinical use.
- Some patients opt for preservation TMS after a year or more, with continued benefits.
Who Should Not Get TMS?
- People with a history of epilepsy or uncontrolled seizures.
- Anyone with implanted metal devices in or near the skull.
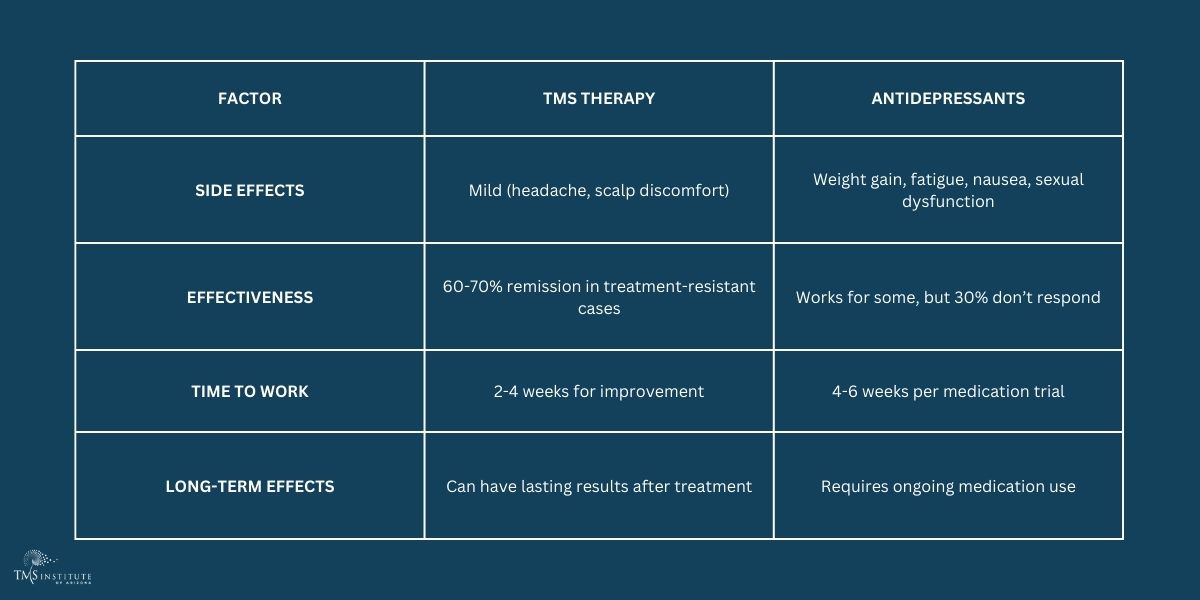
TMS vs. Medication: Which Is Better?
Antidepressants have been the standard treatment for depression for decades. But they don’t work for everyone. In fact, up to 30% of people with depression are treatment-resistant, meaning medications provide little to no relief. This is where TMS makes a difference.
How Do They Compare?
When Medications Fail, TMS Steps In
Most antidepressants work by increasing serotonin, dopamine, or norepinephrine levels. But depression isn’t just a chemical imbalance—it also involves brain connectivity issues. TMS directly stimulates underactive areas of the brain, rewiring circuits linked to mood regulation.
- No daily pills. TMS is a structured treatment course, not a lifelong medication.
- No systemic side effects. Unlike antidepressants, TMS doesn’t affect the entire body.
- No withdrawal symptoms. Stopping TMS doesn’t lead to discontinuation effects.
Can You Get TMS Without a Referral?
Some clinics ask for a referral from a doctor. Others let you schedule on your own. It varies by provider.
When a Referral Is Needed
- If using insurance. Most insurance providers require a formal diagnosis of treatment-resistant depression (TRD) and proof of previous treatment failures.
- If you’re under psychiatric care. Your psychiatrist may need to sign off before starting TMS.
When You Can Start Without a Referral
- If you’re paying out-of-pocket. Private TMS clinics allow self-referral for those who don’t want to wait on insurance.
- If the provider offers direct evaluations. Some clinics provide in-house psychiatric evaluations to determine eligibility.
The best way to know? Call the clinic you’re considering and ask about their process.
Choose the TMS Institute of Arizona for Your Treatment
TMS Institute of Arizona provides expert care using safe and effective technology. Our treatments are proven to help people feel relief. Helping you improve your mental health is our focus.
Why Choose Us?
Our board-certified specialists provide expert care using the most advanced TMS therapy available. Every treatment follows FDA-approved guidelines and is based on the latest research to help patients get the best possible results.
Many people see real improvement, and some even reach full remission. We also work directly with insurance providers to help lower costs. Your comfort, safety, and success matter to us, and we are dedicated to giving you the highest level of care.
You don’t have to settle for medications that don’t work. If you’re ready for a breakthrough, contact us today.
Call now or schedule a consultation online. Your path to relief starts here.
Disclaimer: Medical treatments and conditions vary for each individual. Always discuss any new treatments or concerns with your healthcare provider.