If you’re struggling with depression or other mood disorders and haven’t found success with medications or therapy, TMS may be the breakthrough treatment you’ve been waiting for. At the TMS Institute of Arizona’s Scottsdale location, we specialize in non-invasive, drug-free depression treatment using FDA-approved Transcranial Magnetic Stimulation (TMS). Our compassionate team is here to support your mental health journey with personalized care in a calm, welcoming environment.


Our Scottsdale Providers
Why Choose TMS Institute of Arizona in the Greater Phoenix Area?
- Experienced, compassionate team with board-certified psychiatrists and trained TMS technicians
- State-of-the-art equipment and personalized protocols
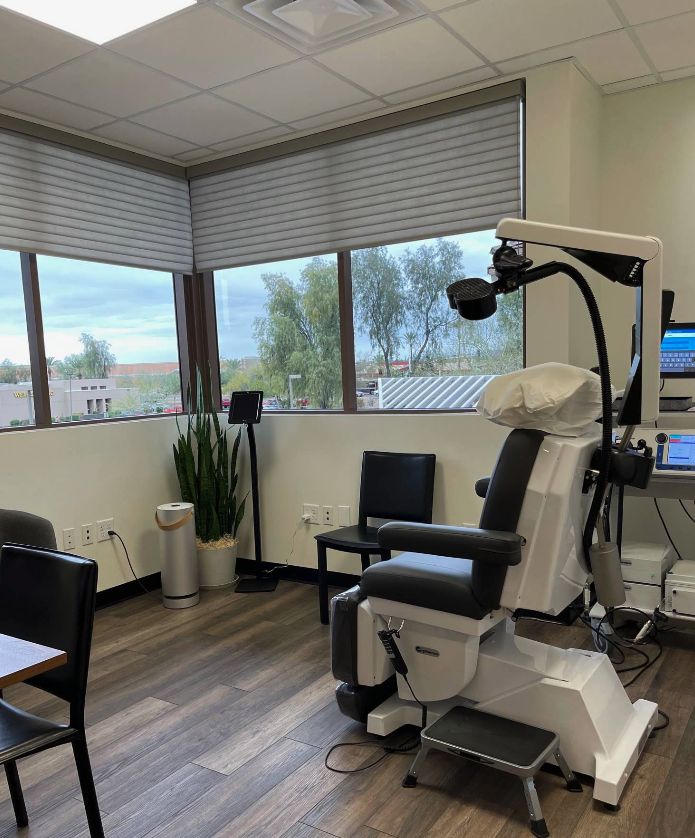
- Comfortable, private treatment rooms designed with your healing in mind
- Local expertise – proudly serving Scottsdale, Fountain Hills, and the surrounding communities for years
Our patients consistently report high satisfaction, improved quality of life, and a renewed sense of hope after completing their TMS treatment.
Finding Our Phoenix Area TMS Clinic
Our Scottsdale clinic is located in a central, easily accessible area serving Phoenix, North Scottsdale, Paradise Valley, Fountain Hills, and the greater Northeast Valley. We’re just off Loop 101 and Shea Boulevard, providing a convenient location for both new and returning patients.
Clinic Details:
- Address: 9746 N 90th Pl, Ste 207 Scottsdale, AZ 85258
- New Patients: 480-448-2916
- Office: 480-668-3599
- Hours: Monday–Friday, 8:00 AM to 5:00 PM
- Parking: Free, on-site parking available
- Accessibility: Wheelchair accessible with private treatment rooms
We encourage prospective patients to first speak to our new patient coordinator to determine if TMS is right for them.